As the fields of health care and public health have been evolving dramatically since the Affordable Care Act, it’s important to take a meaningful look at the progress that partnerships between hospitals, public health, and community stakeholders have made to improve community health. With support from the Robert Wood Johnson Foundation, HRiA recently completed a multi-year study to evaluate the progress of these partnerships. We took an in-depth look at ten sites* around the country to learn about what is working well —with a particular focus on the role of the hospital—and where there are opportunities for growth and improvement. Our goal was to understand the extent to which these partnerships are creating a single, shared community health improvement process among hospitals, health departments, and community organizations to assess and address the needs of the community, including the social determinants of health.
Our learnings demonstrate the valuable and unique role that hospitals can play in community health improvement processes, and also suggest approaches that can make these processes more successful for hospitals and more effective overall. Community health improvement is comprised of the multi-staged process of assessment, prioritization, planning, implementation, and evaluation. The graphic below illustrates that the many partnerships have found strong alignment in the assessment and prioritization phases, but have found challenges and inconsistent alignment during planning, implementation, and evaluation.
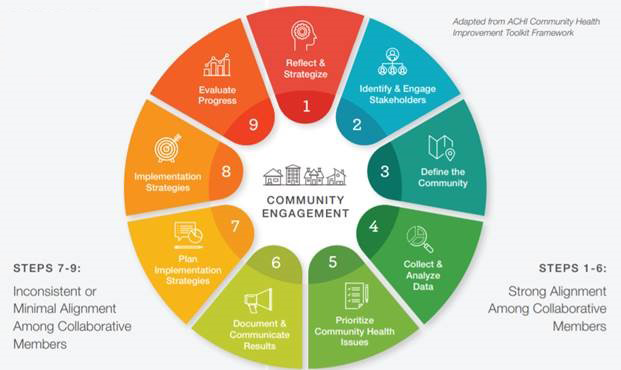
Key learnings
Partnerships come in all shapes and sizes
We visited partnerships that were primarily county-based, serving populations ranging from 60,000 to more than 2 million people. The community health improvement processes we examined are improving alignment of partner efforts and resources within their communities. Alignment is facilitated by developing infrastructures that meet the context, needs, and will of the partners. Each partnership had its own model for how partnerships were structured and how and to what extent partners worked together. In some sites, like the San Francisco Health Improvement Partnership (CA), the partnership is managed by the health department, but does not have a highly formalized structure; while others, like the Health Collaborative of Bexar County (TX), are managed by a separate 501(c)3 organization.
Leadership can vary
Flexibility in how these partners work together is a strong facilitator in the success of these partnerships. The structures through which these partners work together range from non-profit backbone organizations to distributed models where partnership staff are employed by one or more of the partners, typically a hospital or health department. Partnerships serving smaller communities, such as Bowse Health Trust/Rutland Regional Medical Center (VT), tended to have a few staff housed in the hospital or health department. In contrast, partnerships serving larger communities, such as Bexar County, use a non-profit agency as the backbone organization.
Collaborative CHI partnerships are strong and consistent in conducting the assessment and setting priorities
The focus of the partnerships in this study was around conducting a shared assessment, prioritization of community needs, and some planning for implementation efforts to improve community health. Collaborative members work together to meet assessment requirements for their various members, but the collaboratives meet these requirements in different ways. Some partnerships used a coordinated approach and partially shared the assessment and planning process, while others utilized a fully shared or centralized process. For example, the Cecil County, Maryland collaborative (at Union Hospital) has a fully shared, assessment and implementation model where two organizations coordinate all processes with community partners. Partners report that this approach has strengthened their collaboration and ability to leverage resources. In contrast, the University of Pittsburgh Medical Center Children’s Hospital (PA) works with partners, including the local school system, through a highly coordinated, though de-centralized, approach to create healthy schools and students. In this approach, the University of Pittsburgh Medical Center Children’s Hospital conducts its own assessment, planning, and implementation process and reaches out to community organizations and groups for input.
There are many roads to the destination
Partnerships varied in the will and capacity to implement shared solutions to improve community health. Although all partners may not be implementing the same activities together, subsets of partners may be implementing shared activities to address prioritized community needs. In other words, there is no “one size fits all” approach or model to shared strategies to address community health needs. This is particularly true in communities where the number of partners, particularly hospitals and hospital systems, is high. For example, several hospitals in the King County Hospitals for a Healthier Community collaborative (WA) work together through the King County Accountable Communities of Health effort to address many of the priorities identified in the most recent community health needs assessment.
Real outcomes come from a path of policy, systems, and environmental strategies to address social determinants of health
Truly effective partnerships are implementing innovative strategies to address social determinants of health, such as providing mobile food markets and playgrounds to underserved communities (Healthy Baton Rouge, LA), advocating for complete streets policies that increase access to employment and healthy foods for all citizens (Healthy By Design in Billings, Montana), and policy initiatives to limit alcohol availability and increase access to health insurance (San Francisco Health Improvement Partnership, CA).
Take you competitor out for coffee!
Competing hospital systems within a community have learned they can do more together and that they can define where to collaborate and where to compete. In small and large communities, competing hospitals have learned that addressing community health and social determinants needs, such as housing, can reduce inappropriate emergency department use. At the same time, these hospitals can still compete on market share for specific specialty services. We saw this work very well in Billings, MT, where the CEOs of the two major hospital systems realized about a decade ago that both systems and the community would benefit from collaboration among the two systems as well as with the health department, and a Federally Qualified Health Center. These CEOs began meeting regularly in informal settings to discuss areas of collaboration. The CEOs continue to meet this way and can clearly define where they are comfortable collaborating and where they need to compete.
Collective action is just as powerful as collective impact
One of the questions we heard from the partnerships we visited was, should all partners work together on a single strategy to address an identified community health need? In some partnerships, it’s not clear that all partners wanted to work through such a highly coordinated approach.
We’ve all heard the buzz about collective impact and many communities are working on specific efforts where using the five conditions of collective impact makes sense and is appropriate. But not every effort is a collective impact effort and not all communities can achieve it. What’s just as – or even more – important is focusing on collective action through aligning efforts and resources to improve community health. For example, the King County Hospitals for a Healthier Community partners worked to achieve a decrease in the uninsured rate from 43% to 19% following implementation of the Affordable Care Act by working with community organizations and Public Health—Seattle and King County – to develop a network of insurance enrollment navigators.
Build on progress
The ten sites we visited had been working together for at least five years when we conducted our visits. Partners had worked through key issues and their partnership structures had evolved. As the saying goes, “Rome wasn’t built in a day.” Establishing these partnerships takes time and effort. These sites noted it was critical to stop along the way to examine what your partnership has accomplished to build for an even stronger future. The Healthy Choices, Healthy Communities Coalition (HCHCC) is comprised of agencies that serve nine counties in Kentucky, Ohio, and West Virginia. This partnership emerged from two previous entities in the region working on obesity that decided to combine their efforts with the realization that they were competing for the same resources. Now the partners see the bringing together of partners and pooling of resources as a major success.
Get beyond the repetitive assessment cycle
With the 3-year timeline for community health assessment in the IRS requirements, partnership members may think they were just getting traction on some improvement strategies and then they need to turn back to assessment. This challenge can be overcome. The San Francisco Health Improvement Partnership addressed this issue in a recent assessment cycle by doing an “assessment of assessments” and only collecting new data to fill in data gaps. With so many government agencies and national organizations now requiring community assessments, gathering more targeted data with a lighter lift can help partnerships conduct more focused assessment efforts on marginalized groups typically left out of larger community health assessment efforts and can help advance existing initiatives or identify areas for expansion.
The partnerships we examined came together in all shapes and sizes to leverage community context and the needs, will, and capacities of partners to jointly work to improve community health. Although these partnerships have achieved many successes in identifying and prioritizing community needs for health improvement, advancements can still be made, especially in efforts to implement shared improvement activities and evaluate the success of shared efforts. Shared implementation and evaluation is still relatively new territory for these partnerships, leaving room for innovation and new findings that can benefit all collaborative community health improvement efforts.
Resources
*Evaluation sites included:
King County Hospitals for a Healthier Community (WA)
Healthy by Design (MT)
San Francisco Health Improvement Partnership (CA)
The Health Collaborative of Bexar County (TX)
Healthy Baton Rouge (LA)
Healthy Choices Healthy Communities (KY, OH, WV)
Children’s Hospital of Pittsburgh of UPMC (PA)
Union Hospital of Cecil County (MD)
Monroe County Community Health Improvement Workgroup (NY)
Bowse Health Trust/Rutland Regional Medical Center (VT)
Let’s talk community health improvement.
We work with our clients to customize their community health improvement plans to meet their specific organizational and community needs. Reach out if you’d like to learn more. We’d love to hear from you.

