The Community Health Improvement (CHI) process can surface important information and initiate the action needed to create healthy and equitable communities. While most organizations successfully complete their assessments and plans, they often get “stuck” when it comes to prioritization, implementation, monitoring, and evaluation. What strategies can your institution use to successfully complete the full cycle of the CHI process?
Background
The CHI framework as we know it rose to prominence in the mid-1990s by way of the Institute of Medicine Committee on Using Performance Monitoring to Improve Community Health (IOM 1997). Later, the Affordable Care Act (ACA) spurred the IRS to introduce new regulatory requirements for tax-exempt organizations. This included implementing regular community health needs assessments and implementation plans (Cramer 2021) and the introduction of accreditation for local and state public health departments (PHAB).
HRiA’s Approach to Community Health Improvement Work
HRiA’s staff has a long track record of supporting CHI processes in many hospitals and health departments. Health departments and care providers alike maximize the benefits of CHI work when they invest in the full cycle of the process. As seen in Figure 1, HRiA’s Approach to CHI work comprises six steps:
- Assessment
- Prioritization
- Planning
- Implementation
- Monitoring
- Evaluation
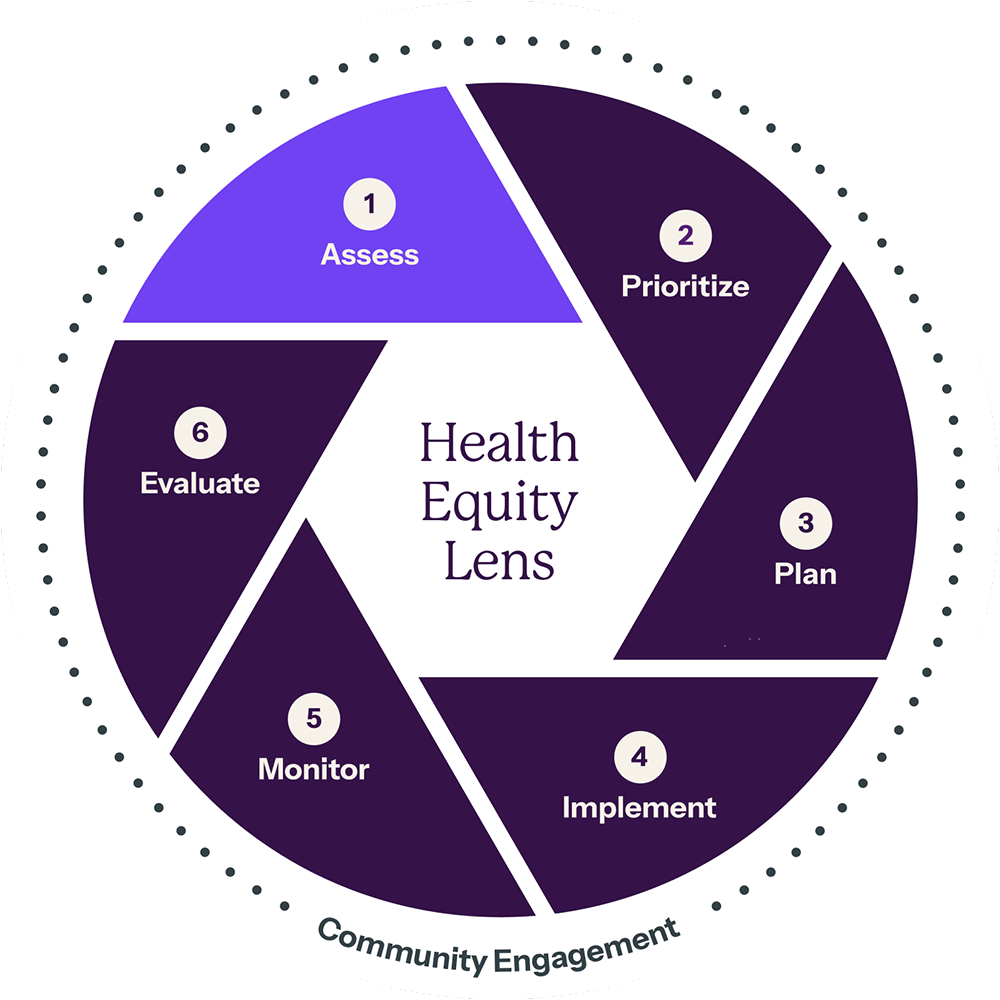
Each of these steps builds upon the previous step, creating a comprehensive and intentional process with health equity at the core. Community engagement is the essential element at each phase of the CHI process. Integrating community engagement and leadership ensures health equity is a focus and outcome of CHI work. As our framework demonstrates, HRiA’s approach to CHI reflects a deep commitment to equitable community engagement. (See our approach in action.)
Sticking Points
CHI work often stagnates after planning. Four of the most common reasons include:
- Inadequate time and resources
- Insufficient community engagement
- Unclear systems of accountability
- Lack of integration with practices and systems
Does this describe your institution? Here are a few practical strategies to support completion of the CHI cycle:
Inadequate time and resources.
Community engagement is rarely (if ever) the only initiative underway at any moment. Like any other effort, community engagement work vies for limited resources. Even if financial resources are not a limiting factor, time certainly is. Strategic plans only last for three to five years, and organizational and community leaders have competing priorities; additionally, CHI work is often added to plates without adjusting other priorities. What do you do when your team or institution does not – or cannot – allocate sufficient time or resources to conduct deep, continuous community engagement?
STRATEGY: Provide sufficient resources (including dedicated time and funding) for staff and community leaders conducting CHI work.
Community members are essential to successful CHI work. Engagement starts at the beginning; it both informs and integrates with the methods and approaches outlined in the assessment, continues as appropriate through each phase, and influences planning for the next round of the cycle. Ensure that you factor in fair compensation for the time and the lived experience of community members and the staff who work with them. This means meeting residents where they’re at and when they’re available, providing translation services, and rebalancing responsibilities—during AND beyond the assessment phase.
Insufficient community engagement.
Improving community health requires deep, authentic, sustained community engagement. By limiting your engagement to the people that you work with regularly in the assessment and planning processes or relying on secondary data, you are likely missing the voices of those most impacted. Offering limited options for participation or failing to follow up in future phases can damage relationships with the community. How can you deepen your community engagement work efficiently and effectively?
STRATEGY: Create varied and recurring opportunities for power shifting and decision making.
Community engagement that considers the different needs within the community can increase the likelihood of your CHI work creating impact. Identify opportunities for sustained engagement throughout the process, such as multiple community meetings at a variety of times (considering varying work and caregiving schedules of participants). Collaborate with existing coalitions and community groups to reach folks in places where they already congregate.
Ultimately, the community should strongly influence the selection of priorities based on what is important and relevant to them, as well as the development, implementation, and improvement of the strategies put into place. Use the community engagement continuum to explore how you might lift up community voice and incorporate public participation strategy
Unclear systems of accountability.
Generating community impact requires collective effort within complex institutions and among diverse stakeholders. Typically, a single unit is not responsible for all parts of the CHI process. However, the work can end up falling on the shoulders of one individual or department, or tasks can be lost in the shuffle of unclear systems of accountability, drastically limiting your potential impact.
STRATEGY: Coordinate communication among partners.
When partner engagement is done well (authentically and sustained), your hospital or health department will not be solely responsible for all CHI work. Careful coordination of communication and outreach is needed when there are multiple stakeholders responsible for the plan. Defining roles at the project outset, as well as setting a schedule for regular monitoring and reporting are critical steps to ensuring accountability, continuous buy-in, and impact.
Lack of integration with practices and systems.
Hospitals and health departments often struggle to implement a plan that is not sufficiently integrated with their other work, does not have internal and external investment and support, and is not regularly monitored and reported.
STRATEGY: Integrate with existing practices and systems.
Thoroughly integrating CHI work with other critical work will ensure that the work gets done. Identify areas where CHI work intersects with existing practices and systems. Look into other initiatives happening in your community and identify places where you might collaborate on data collection, engagement, dissemination, and more. Considering existing avenues can streamline your work and build stronger partnerships with anchor institutions and community members.
Next steps
The CHI process offers an opportunity to create healthy, equitable communities. Authentic, sustained community engagement throughout the CHI process is critical to success. Pour the time, dedication, care, and feeding into your process and the impact will be worth the effort.
Learn more about HRiA’s CHI work and team.
Want to borrow our lens? Connect with us.
Suggested citation: Community Health Improvement Lens (2024), illustration by Health Resources in Action.
