Our Work
We are a national organization working locally. Discover how we and our partners are creating real sustainable impact.

Our Impact in 2024
82,157
Calls, chats, and texts to Helplines
$21M
Dollars distributed through HRiA’s grant programs
213
Awardees of HRiA’s grant programs
Featured Impact Story

Assessment & Planning
Collaborating on community health improvement
With several shared challenges, two neighboring Massachusetts towns sought to collaborate in their community health improvement efforts. Together with HRiA, they pursued a joint community health assessment and plan. Discover how HRiA’s process guided the team in identifying common needs and co-creating clear, actionable plans to improve the health of both communities.

Assessment & Planning Capacity Building Policy & Systems Change
Advancing health equity at the local level
Lincoln County Health and Human Services (HHS) in Oregon partnered with HRiA to advance equity within their department. Grounded in HRiA’s Health Equity Framework, this work aligned Lincoln County HHS’s culture and practices with its goals of positive, equitable health outcomes for its community. Representatives from the team went on to present their findings at the 2023 NACCHO 360 conference. Join us on the journey from local health department to national stage in our impact story.

Capacity Building Grantmaking
Combatting racism through community-centered investments
Since 2020, Massachusetts organizations have leveraged an unusual yet powerful resource to disrupt outdated systems and build something that works. Learn about strategic investments across the state and their collective efforts to shift the narrative in our story about the MA Community Health and Healthy Aging Funds (aka The Funds).

Capacity Building
Diversifying the STEM workforce through youth development
The Leaders through Education, Action, and Hope (LEAH) Project engages youth of color in exciting hands-on STEM experiences and college readiness programming. In its 20 years, LEAH has helped nearly 100% of participants gain the leadership skills they need to succeed. Read on to learn how this groundbreaking Boston-based program develops future STEM superstars.

Grantmaking
Funding innovations in the treatment of human disease
The Charles A. King Trust Postdoctoral Fellowship Program supports early-stage researchers at a critical juncture in their career - the postdoctoral stage. Since 1958, this prestigious program has funded nearly 1,000 promising scientists as they transitioned from trainee to independent investigator. Read on to learn about the legacy—and the future—of the King Fellowship program.
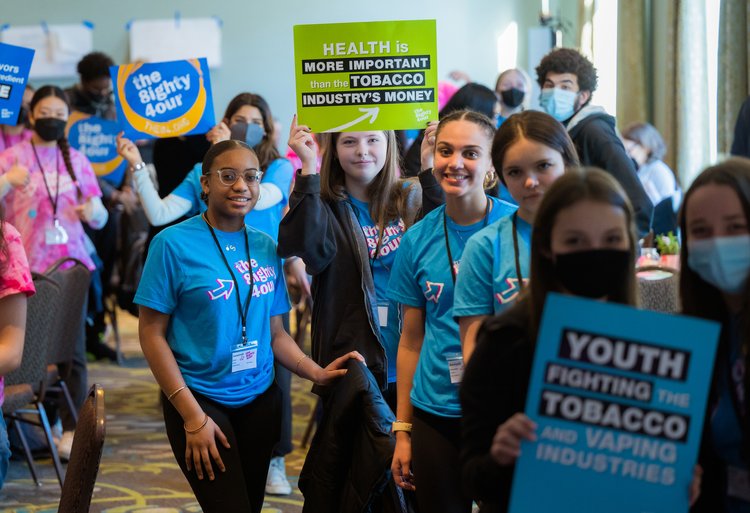
Policy & Systems Change
Centering youth and community voice to fight the tobacco industry
For decades, HRiA and partners have worked to counteract tobacco-related harms. Below, we share three examples, including the youth advocacy of The 84 Movement, the progressive implementation of smoke-free housing policies in Boston, and the community mobilization that resulted in the statewide ban of flavored tobacco and vape products. Collectively, these policy, systems, and environmental (PSE) change approaches result in meaningful, ongoing community and statewide impact.

Assessment & Planning
Collaborating on community health improvement
With several shared challenges, two neighboring Massachusetts towns sought to collaborate in their community health improvement efforts. Together with HRiA, they pursued a joint community health assessment and plan. Discover how HRiA’s process guided the team in identifying common needs and co-creating clear, actionable plans to improve the health of both communities.
Let’s make impact together.
We work with our clients to create custom solutions that meet their organizational and community needs. If you want to explore how we might work together, we’d love to hear from you.